DR ROSIE STOKES of DDRC Healthcare looks at a very recent “drowning from the inside” case study – with thanks to UK diver SALLY DE COURCY for sharing her story

Immersion pulmonary oedema has been a hot topic for us of late. The symptoms of IPO remain poorly recognised among divers, open water swimmers and even healthcare professionals, resulting in serious injury or even death.
Also read: Good Samaritan divers break out O2 in Co-op
As one of DDRC’s dive doctors, I cover the British Hyperbaric Association diver helpline and respond to dive emergencies, providing specialist input and advice where needed.
On this occasion I was called by the Coastguard to provide support for a diver unresponsive on the surface of the water.
The diver was evacuated to A&E, and I met her there on arrival. Sally has been kind enough to share her story:
Also read: Snorkel-deaths report questions IPO findings
“On my past few diving holidays, I had noticed that I started coughing frequently on the dives and put this down to my throat feeling dry. I had also become more aware of my breathing, as if I couldn’t get quite enough air, but as my equipment was working and I was in good health I decided that this must be in my imagination.”
“However, these feelings were making me increasingly apprehensive, and detracted from the pleasure of diving. On two previous occasions, once before the pandemic and then in the Philippines in April this year, I had come up to the surface feeling short of breath, with a tightness in my chest, which was very alarming.”
“However, once out of the water and having taken off my wetsuit, these symptoms disappeared. My husband Andy (dive-buddy) and I decided that maybe I was anxious and hyperventilating, although I didn’t feel anxious at the time, but we couldn’t think of any other cause. Neither of us had ever heard of IPO.”
‘At around 13m I felt short of breath’
“On 9 July, 2023, I was diving from a dive-boat with a group of friends from BSAC in the Scilly Isles. It was my first dive on this trip, and my 30th dive in 2023. I had previously done around 100 dives. I was wearing a new semi-dry wetsuit that had been professionally fitted.
“At around 11am, after doing our buddy-check, Andy and I started our first dive. The water was calm, not choppy. After a necessary weight-adjustment for my new suit, we got down to around 5m and I felt that my regulator might not be working, as I had mild shortness of breath. I indicated that we needed to go back up to the surface.”

“At the surface, I checked the regulator and decided to try again. At around 13m I felt short of breath. I indicated that I wanted to abort the dive but, having checked that the cylinder gauge had gone down and that I must be getting air, I decided all was well.”
“Cross with myself and determined to overcome what I thought must be anxiety due to increasing diving apprehension, I indicated to Andy that we could continue.”
“We descended to the seabed at 25m and Andy inflated our SMB. We then swam towards the reef, ascending slightly, and I was aware that I was very short of breath. I felt as if I couldn’t get enough air into my lungs.”
“At 13m I indicated that we needed to go up. Andy gave me the OK sign and was winding in his SMB reel. I became increasingly short of breath and thought I was going to drown. In hindsight, Andy was not aware of the urgency, still attributing my symptoms to anxiety.”
“We then began our ascent. At about 6m, we attempted to do a safety-stop. As I was doing this, I realised that I could no longer understand my dive-computer and that I was extremely confused. Understanding the danger of this, I indicated that I was going up, and Andy followed.”
“When I got to the surface, I couldn’t breathe and took the regulator out of my mouth, desperate to draw in air, but nothing happened. I felt as if the BC was constricting my chest and, in my confusion, I deflated it, believing that this was causing the feeling of my chest being squeezed.”
“Meanwhile I saw Andy and called out: ‘I can’t breathe!’ twice. I lay back, desperately trying to get air, and that was the last that I remember. Apparently I then became unconscious, my head going under water because of the deflated BC.”
Helpful past experiences
“There are a few things that helped me to stay composed in the water during a frightening experience. Nine months earlier, while walking in Snowdonia, I fell 40m. Having landed in an icy stream, and sustaining multiple injuries, I found out later that I was hypoxic.”
“While in the water I had been able to recognise the signs of hypoxia (confusion) and knew it was critical that I got to the surface.”
“I had received cognitive behavioural therapy (CBT) for PTSD because of the walking accident. Part of CBT was to consider all possible outcomes, and what you need to do to attain the most favourable.”
“Before confusion set in, I used these CBT skills to understand that it was imperative to keep calm in the water to reach the surface. It helped me to process that my equipment was working and that there must be something medically wrong.”
“Trying Andy’s octopus would not help but might put me at risk of drowning when I took the regulator out of my mouth if I responded to the overwhelming need to draw air.”
“Ironically, I am quite sure that if I hadn’t experienced the Snowdonia fall, I might not have survived this incident.”
“It is important to me that divers become aware of the risk of IPO, which carries a risk of fatality. I hope that by sharing not only how it felt in the water on this occasion, but also the symptoms that I had experienced leading up to it, on previous dives, that it might alert divers to seek medical help as soon as they experience any symptoms.”
“I was lucky enough to be admitted to Derriford Hospital in Plymouth, and I am indebted to the excellent care that I received from DDRC – many thanks.”
Causes and effects
Sally was extremely lucky to have survived this incident. The Coastguard reported that she had been in respiratory arrest on the boat, and the quick actions of her husband and the boat-skipper saved her life.
Immersion pulmonary oedema is caused by the pressure effects of being submerged in water, with the greatest immersion effect seen at the surface.
This, in combination with various contributing factors such as over-hydration, a tight wetsuit and being in cold water, as well as underlying physiological changes in the body as we age (high blood pressure), can be enough of a provocation to overwhelm the heart and lungs and cause fluid (oedema) to accumulate in the airways.
As you can imagine, this feels as if you are drowning, and you might start to cough up blood-stained frothy sputum.
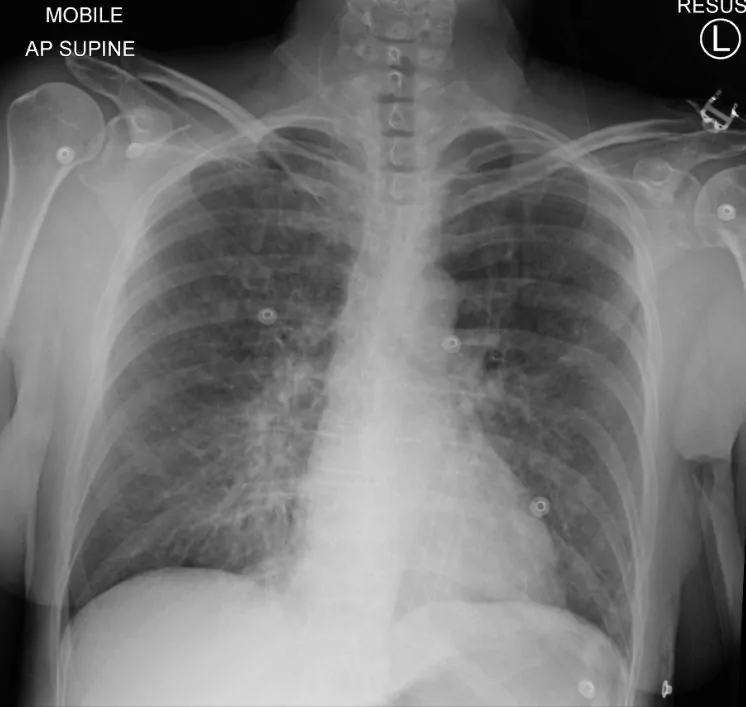
It is important to say that IPO is a rare condition. However, if you do experience any shortness of breath that is out of the ordinary while diving, the most important thing to do is to get out of the water safely.
Of course, this is much easier at the start of a dive, so it is vital not to ignore any symptoms on the surface.
Once you are on dry land the symptoms will settle with time – remove any tight clothing and keep warm, and contact a medic if you feel unwell or remain short of breath.
Discuss these symptoms with a suitably qualified healthcare professional before you return to diving.
If you are with a diver who is unwell and you think might have IPO, get them out of the water and on some oxygen to help them breathe, and call the emergency services. They should be taken to an A&E for assessment and support for their breathing.
In the UK, the British Hyperbaric Association (BHA) Helpline is available 24/7 for advice if you are unsure of what to do – call 07831 151 523 (Scotland 0345 408 6008)
If you would like to know more about IPO, DDRC Healthcare has a section on its website: Can I Dive With A History Of IPO?. Or check out the UKDMC website: Immersion Pulmonary Oedema.
DDRC Healthcare is a Plymouth-based not-for-profit organisation and UK charity specialising in diving medicine, hyperbaric oxygen therapy and medical training.
Also on Divernet: DDRC needs divers’ help on lungs, Breathless swimmer’s case boosts IPO awareness, Red flags for snorkellers: how to stop the quiet deaths
